DIEP Flap Technique for Umbilicus Reconstruction
Brian B, Waqqas J and Wojciech D
DOI10.21767/2471-9943.100038
Brian B, Waqqas J and Wojciech D*
Department of Plastic Surgery, Lenox Hill Hospital, New York, NY 10075, USA
- *Corresponding Author:
- Wojciech D
Department of Plastic Surgery, Lenox Hill Hospital
New York, NY 10075, USA
Tel: (212) 390-8400
E-mail: drdec@drdec.com
Received Date: May 02, 2017; Accepted Date: May 23, 2017; Published Date: May 29, 2017
Citation: Brian B, Waqqas J, Wojciech D. DIEP Flap Technique for Umbilicus Reconstruction. Colorec Cancer. 2017, 3:1. DOI: 10.21767/2471-9943.100038
Copyright: © 2017 Brian B, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
This article describes a new perforator flap technique for reconstruction of the umbilicus. Previously described techniques for umbilicus reconstruction are not satisfactory because of their aesthetic limitations. Namely the need for incisions outside of the reconstructed umbilicus; limited depth of the reconstructed umbilicus; or reliance on skin grafting, which results in a scarred and contracted umbilicus. All of these limitations are eliminated by utilizing a perforator flap for umbilical reconstruction.
Keywords
Umbilicus reconstruction; Abdominoplasty; DIEP flap
Introduction
The loss of a native umbilicus is occasionally encountered following abdominoplasty or abdominally based autologous breast reconstruction. This complication is especially common in the setting of an umbilical hernia. In cases where preoperatively there is a high suspicion for loss of the umbilicus, a deep inferior epigastric artery perforator flap is designed based on one of the periumbilical perforators. This can be done safely and easily in the setting of unilateral DIEP flap breast reconstruction or abdominoplasty, and with more careful planning in the setting of bilateral DIEP flap breast reconstruction.
Surgical technique
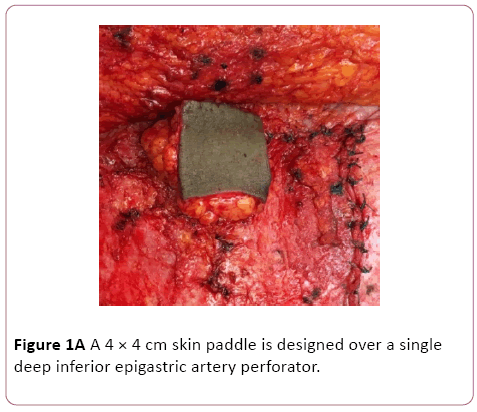
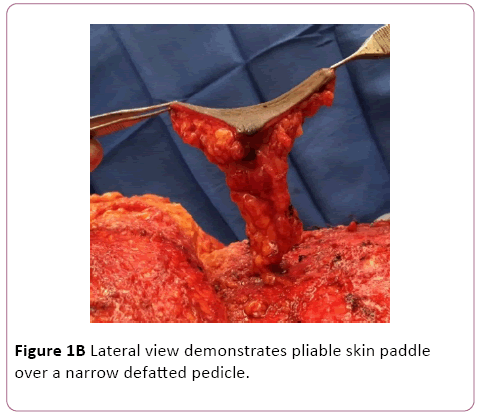
During abdominoplasty or DIEP flap elevation a periumbilical perforator is identified. A 4 × 4 cm area of overlying skin is marked and incised. In cases of abdominoplasty or unilateral autologous breast reconstruction the skin paddle is designed over tissue destined to be discarded. Depending on breast reconstruction volume requirements this may or may not be feasible in bilateral breast reconstruction cases. The intervening tissue between the origin of the perforator at the level of the fascia and the skin is aggressively defatted. This step does not require any perforator dissection and is done quickly with a curved mayo scissors. The resulting skin flap has an adequate surface area of pliable skin based on a narrow and very mobile pedicle (Figure 1A and 1B). Tissue viability is assessed by observing the punctate bleeding from the skin edges.
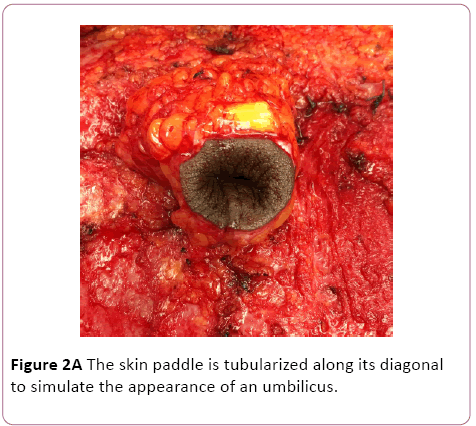
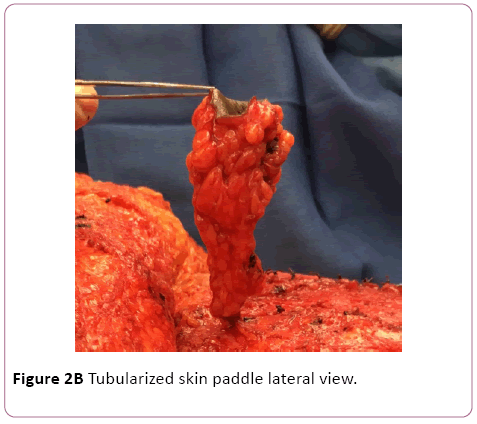
The skin paddle is tubularized along its diagonal, and a vertical seam is created inferiorly by sewing two adjacent edges of the square. Excess skin is removed from the superior corner of the tubularized flap. This creates an inverted skin cone, which at this stage closely resembles a native umbilicus (Figure 2A). Care is taken to maintain the orientation of the flap because twisting and vascular occlusion is a risk with the narrow base of the flap (Figure 2B).
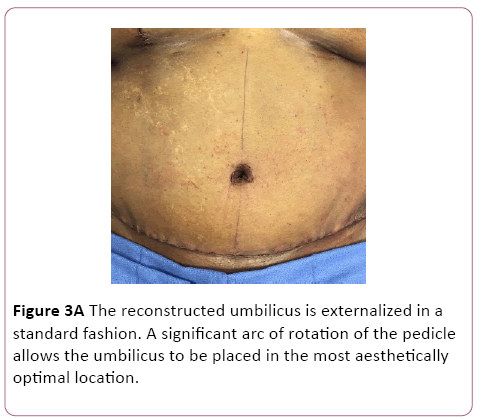
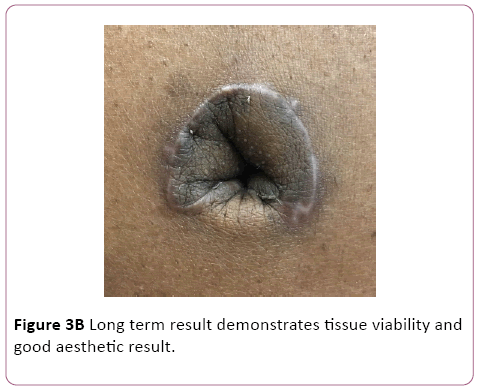
The umbilicus is externalized in a standard fashion. A significant arc of rotation of the flap pedicle allows freedom to place the umbilicus in an aesthetically optimal location. It is the authors preference to reconstruct the umbilicus by incising an inverted U in the abdominal skin, and defatting the underlying tissue. The inverted U flap is then inset into the seam of the tubularized perforator flap (Figure 3A). Scars are limited to the perimeter of the reconstructed flap; the inferior edge of the reconstructed umbilicus appears scarless. Long term results are aesthetically pleasing, with limited scars, and an adequate depth of the umbilicus (Figure 3B).
Discussion
Reconstruction techniques described in the literature have included skin grafting, purse-string suture, cartilage, and flaps [1-4]. To our knowledge this is the first technique described in the literature where a neoumbilicus is created using a deep inferior epigastric artery pedicled perforator flap. The reconstructed umbilicus has a natural morphology, with adequate depth, limited scars, and is free from the tissue contracture associated with skin grafts. The relatively long pedicle length should allow umbilical reconstruction to be performed even in the setting of more extensive ventral hernias which require myofascial releases, although this has not yet been attempted by the authors. This technique is limited to cases of immediate umbilicus reconstruction where there is a preoperative concern for loss of the native umbilicus, and is not suited to secondary umbilicus reconstruction for obvious reasons. Long term results demonstrate longevity of the umbilical reconstruction. We consider this technique our preferred method for umbilicus reconstruction.
References
- Joseph WJ, Sinno S, Brownstone ND, Mirrer J, Thanik V (2016) Creating the perfect umbilicus: a systematic review of the recent literature. AesthPlastSurg 40: 372-379.
- Malic CC, Spyrou GE, Hough M, Fourie L (2007) Patient satisfaction with two different methods of umbilicoplasty. PlastReconstrSurg 119: 357-361.
- Lee MJ, Mustoe TA (2002) Simplified technique for creating a youthful umbilicus in abdominoplasty. PlastReconstrSurg 109: 2136- 2140.
- Hazani R, Israeli R, Feingold RS (2009) Reconstructing a natural looking umbilicus: a new technique. Annals of plastic surgery 63: 358-360.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences